Texas is poised to implement stringent new regulations on ketamine, a fast-acting sedative increasingly used to treat mental illness, sparking a fierce debate between medical authorities advocating for patient safety and providers concerned about limiting access to a vital therapy.
The proposed rules, which include heightened physician oversight during administration and a ban on in-home use, are slated for publication on May 8, with the Texas Medical Board scheduled to vote on the changes in June.
The move comes amid a surge in ketamine’s popularity, driven by its efficacy in treating conditions like depression and PTSD, but also by its easy accessibility through telehealth prescriptions and medical spas.
This widespread availability has raised alarms among regulators and some medical professionals, who point to the drug’s potential for abuse and severe side effects. The death of actor Matthew Perry, linked to ketamine, has further amplified public awareness of its dangers.
Data from poison centers nationwide reveal a concerning trend, with ketamine poisonings more than doubling since 2019 to 414 in 2023. Texas itself has seen a steady increase in ketamine-related calls to poison centers, rising from 15 in 2020 to 40 in 2024.
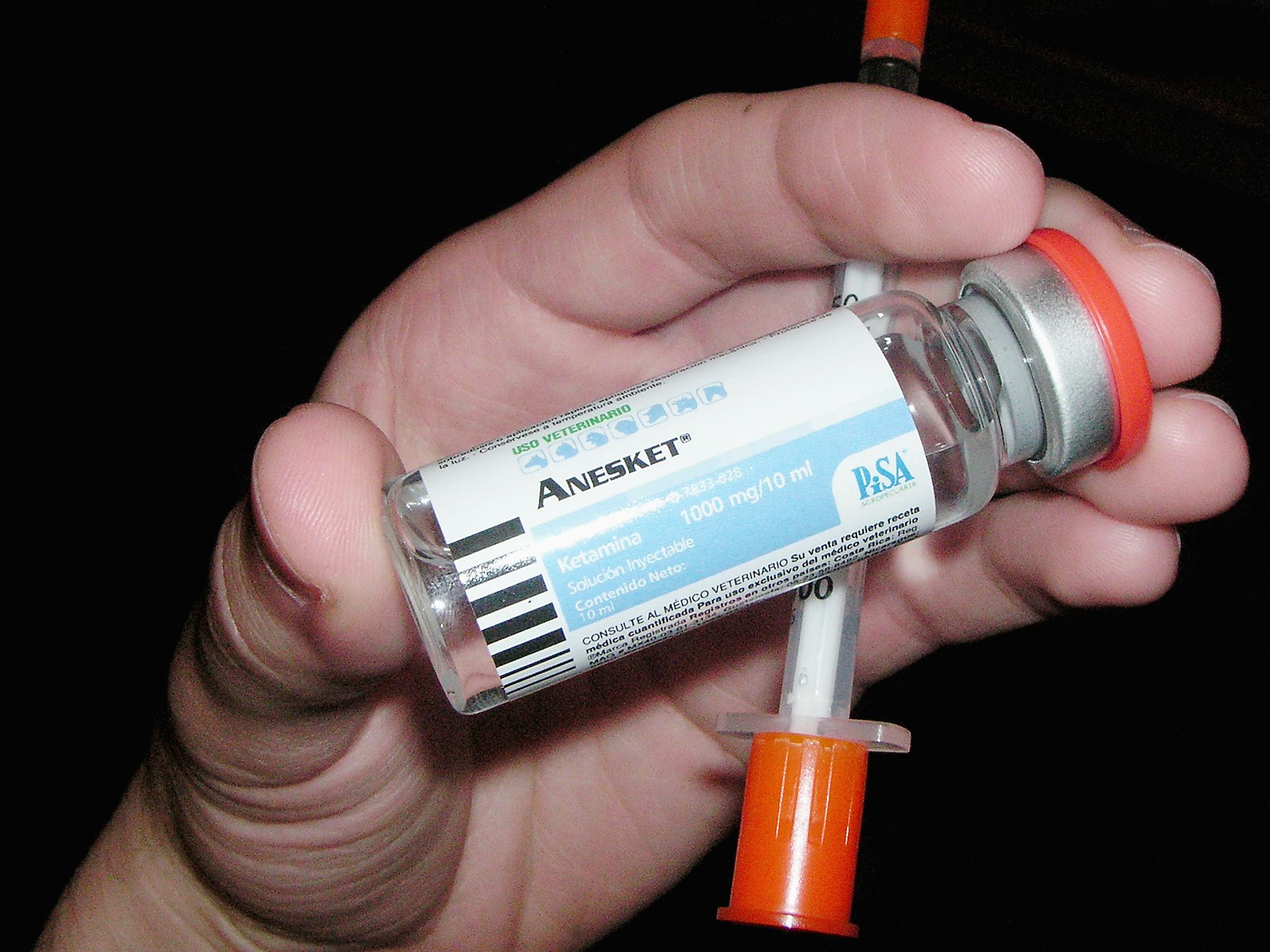
Currently, many ketamine clinics in Texas operate with a physician on staff but rarely on-site, with advanced-practice registered nurses (APRNs) and certified registered nurse anesthetists (CRNAs) often overseeing multiple treatments simultaneously.
The proposed regulations aim to address this by requiring that if a physician is not on-site, medical staff cannot administer ketamine to more than two patients at a time. Furthermore, the rules prohibit ketamine treatments outside of registered clinics, effectively banning in-home use, and mandate that health providers complete mental health treatment training before administering the drug.
Supporters of the tighter controls emphasize the drug’s potency and the critical need for proper administration. Rep. Tom Oliverson, an anesthesiologist and former medical board member, stated, “People think ketamine is a wellness treatment when it’s not.
Everyone wants a miracle cure. But the reality is this is a dangerous anesthetic.” He questioned, “So then the question is, who should be allowed to administer those things so that it’s done safely?” Spencer Miller-Payne, a spokesperson for the Texas Medical Board, underscored the drug’s unique risks: “Due to its potency, proper administration methods are essential. Ketamine, unlike opioids, cannot be counteracted by other medications like Narcan.”

He added that the board seeks to ensure patient safety without unduly restricting access to care. Mary Moore, owner of Lake Austin Psychotherapy, believes stricter regulations could help “legitimize” ketamine therapy, making it more acceptable to insurance providers. She also expressed concern over the “conveyor belt model” of some clinics, where psychotherapy is often overlooked.
However, industry leaders and non-physician medical providers are vehemently opposing the proposed changes, arguing they will severely limit access to care and disproportionately affect vulnerable patients.
They contend that forcing clinics to choose between hiring an expensive on-site physician or drastically reducing patient numbers will raise treatment costs by $300 to $500, making it unaffordable for many.
Alli Waddell, CEO and co-founder of Austin ketamine clinic Illumma, called the proposal “insulting” to APRNs, stating, “It doesn’t make sense. Nurse practitioners are running the entire intensive care units with 25 patients who are very sick, and they are comfortable with them doing that, but they can’t be in a space with a very safe drug?”
She believes the regulations are a “power grab” by physicians under the guise of patient safety, designed to “gut the industry” and force clinics to shutter.
Ketamine therapy, when used in a clinical setting and paired with counseling, is considered one of the safest and most effective treatments for severe, treatment-resistant mental illnesses such as depression, PTSD, and suicidal ideation.
It works by helping to repair brain connections often damaged by mental illness, making the brain more “malleable for change,” as described by Will Ratliff, director of operations at Transcend Health Solutions. However, providers acknowledge its high potential for dependency and risks of cardiovascular strain, respiratory depression, and organ damage with long-term misuse.
Bradley Armendariz, a licensed professional counselor who provides ketamine treatments, emphasized, “You can’t just take ketamine and fix your life. You will feel temporarily good and then go back down. It still requires work and action on the client’s and the mental health providers’ part, too.”
Critics also highlight that many ketamine clients are low-income and highly suicidal, unable to bear the financial or mental burden of increased costs. The ban on in-home use is particularly concerning for rural patients, who often rely on telehealth due to physician shortages in their communities.
Leonardo Vando, medical director of Mindbloom, noted, “We have a lot of our patients from Texas. Most of them choose at-home. Not because they are choosing between us and in-person, but because we are their only option within a span of two hours.”
The regulatory framework established in Texas is expected to serve as a model for other states, making the outcome of the June vote nationally significant. Will Ratliff warned, “This is going to radiate throughout the entire nation, and there’s literally only a handful of people fighting for it. Physicians are actively shutting down the practice of something that saves a lot of lives just because of ignorance.”
The debate ultimately centers on balancing the critical need for patient safety with ensuring continued access to a potentially life-changing, yet potent, medical treatment.
