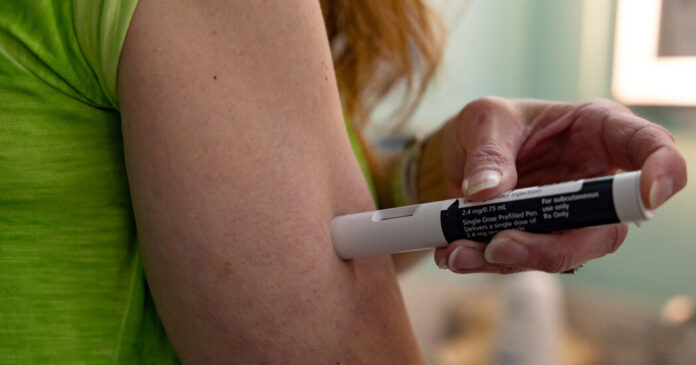
Millions of older Americans may have access for the first time to obesity drugs at a low price of $50 a month starting in July under a Medicare pilot program.
While Medicare Part D already covers some GLP-1 medications for conditions like diabetes, cardiovascular disease and sleep apnea, the government program for people 65 and older had prohibited coverage solely for obesity. Now, more people on Medicare will be eligible, including those who are most overweight and those with both obesity and conditions like prediabetes or uncontrolled hypertension.
The $50 monthly price — which will cover any dosage amount — is much lower than what Medicare patients currently pay out of pocket for GLP-1s.
About 40 percent of the 70 million people enrolled in Medicare meet the clinical definition of obesity, data from the Centers for Disease Control and Prevention shows. The Congressional Budget Office estimates that 29 million Medicare beneficiaries would then qualify for GLP-1 drug coverage, although 16 million already have access for conditions such as diabetes or cardiovascular disease.
But many older people may not be able to afford an extra $600 a year for another prescription, as they are already struggling with rising health care costs. KFF, a health research organization, reported that one in four Medicare beneficiaries had an income below $24,600 in 2024, and that half lived on incomes below $43,200.
Another concern is whether the program would extend beyond 2027. Although the pilot could be continued, adding the benefit permanently would require a change in federal law and agreement among health insurance companies to offer the medications in Part D prescription drug plans.
The financial burden for Medicare is another consideration if such coverage were extended. The C.B.O. estimated that adding weight-loss drugs would cost Medicare $35 billion from 2026 to 2034. A spokesperson for the Centers for Medicare and Medicaid indicated that the agency had not publicly released cost estimates on either the pilot, called the Medicare GLP-1 Bridge program, or the permanent model.
Here is what Medicare beneficiaries seeking coverage need to know about the pilot program.
Who can participate?
Those eligible include not only enrollees who are 65 and older but also Medicare beneficiaries with disabilities.
The Bridge program is temporary, open mainly to people already enrolled in either the Part D prescription plan or the private Medicare Advantage plans that include drug coverage. But your Part D provider will not offer coverage.
“Your Part D plan will have nothing to do with making decisions about whether or not you can access a GLP-1 under the Bridge model,” said Juliette Cubanski, deputy director of the program on Medicare policy at KFF.
Instead, a health care provider must determine whether you meet the Bridge program’s clinical requirements, which are based on body weight and health status. Patients with a body mass index of 35 or higher will qualify; those with a lower B.M.I. may also qualify if they have been diagnosed with other related conditions.
Providers will need to submit a prior authorization request and a prescription to Humana, which will be processing requests.
If the request is approved, you can fill the prescription at any pharmacy. The list of GLP-1s that can be prescribed for obesity includes Eli Lilly’s Foundayo and Novo Nordisk’s Wegovy in injectable and tablet forms; and Lilly’s Zepbound KwikPen.
If you are taking a GLP-1 drug for a different condition, such as diabetes, that will continue to be covered by your Part D plan.
What will this cost?
The $50-a-month co-pay is separate from any premiums or deductibles you pay for Part D. Because Bridge purchases are processed outside Part D, the monthly cost does not count toward Part D deductibles or out-of-pocket spending limits.
Older people with very low incomes typically qualify for assistance with Part D costs through a federal program called Extra Help, which subsidizes premiums, deductibles and cost sharing. That assistance will not be available because the program runs outside Part D.
Those who have both Medicare and Medicaid coverage and are not required to make co-payments — or minimal ones at most — would be eligible. But the $50-a-month price would apply to them, too.
“It could be difficult for low-income and modest-income older adults to participate and take advantage of the new coverage,” said Ramsey Alwin, chief executive of the National Council on Aging.
State Medicaid programs already have the option of covering GLP-1 drugs for obesity treatment, but only about a dozen states do so, according to KFF.
Why is this outside Part D?
Federal law prohibits Medicare from covering medications prescribed specifically for weight loss; making GLP-1 coverage permanent would require an act by Congress. In the meantime, C.M.S. has the legal authority to run time-limited “demonstration projects” to test new payment or coverage approaches like this one.
The federal government had aimed to move the weight-loss drug coverage from its pilot to Part D in 2027. But health insurance companies balked because of the potentially high costs of covering enrollees and a lack of data for determining the number of patients that would guide their pricing plans next year, said Kylie Stengel, principal at Avalere Health, a research and consulting company.
“There’s really no historical data on GLP-1 use for obesity in Medicare, and insurance plans really need that data to assess that risk so that they can accurately set plan prices,” she said.
Will I still be able to get the drugs after the pilot ends?
It is an important question, because research shows that most people need to stay on the drugs to maintain weight loss or other health benefits. There is no clarity on next steps, Dr. Cubanski of KFF said. Much will depend on whether C.M.S. can persuade more insurance plans to participate.
“The really big question is what happens at the end of 2027 if C.M.S. isn’t able to stand up this model in Part D,” she said.
Even if Part D does permanently cover the GLP-1s for weight loss, some people will not be able to afford the drugs. Cost-sharing is expected to increase above the pilot’s monthly fee of $50.
One recent University of Pennsylvania study found that monthly cost-sharing for GLP-1 drugs already covered by Part D ran as high as an estimated $167 a month last year.
“I’d expect similar costs for the weight-loss drugs, and maybe higher,” said Matthew Klebanoff, an assistant professor of medicine at the University of Pennsylvania and an author of the study.
Polling by KFF found that over half of GLP-1 users said these drugs were difficult to afford, and one in four said they were “very difficult” to afford.
The price of these drugs makes forecasting uncertain. Drug manufacturers agreed to supply the weight-loss drugs to Medicare enrollees at a net price of $245 a month — a steep discount compared with prices in commercial markets.
Also uncertain is how much Medicare might save over time, when taking into account the potential for reductions in obesity-related health conditions, including metabolic, cardiovascular and respiratory illnesses. The C.B.O. estimate included $3 billion in savings over that period — but that figure may be conservative.
One group of researchers projected savings of $18 billion over a 10-year period. “We found large downstream reductions in the rates of diabetes and cardiovascular disease, in particular,” said Elbert Huang, a professor of medicine at the University of Chicago and co-author of the study.
The affordability issue — coupled with uncertainty about whether the pilot will lead to permanent coverage under Part D — worried some experts. Millions of older people might start GLP-1 treatment for obesity but then be suddenly cut off.
“There’s a great deal of concern about people having yo-yo experiences with GLP-1 drugs,” Dr. Huang said. “When people stop treatment, they not only regain the weight they had lost — but the weight they put back on is predominantly fat.”
“We’re about to do a giant national experiment on older adults in America,” he added.